Summary:
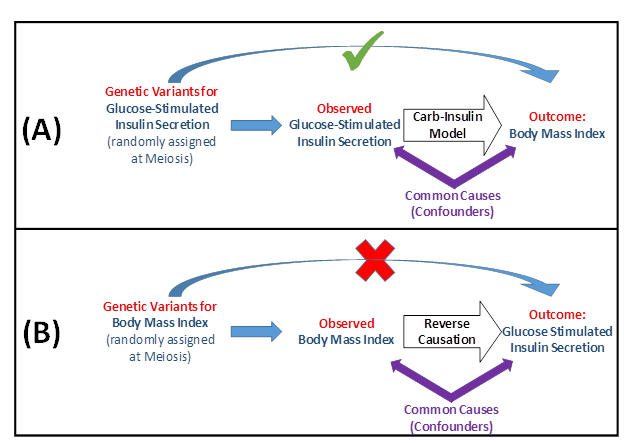
The carbohydrate-insulin model of obesity postulates that increased insulin secretion in response to a high glycemic load diet drives excess weight gain. Because of the close interrelationship between obesity, insulin resistance, and hyperinsulinism, however, investigating this hypothesis is often complicated by possibilities of confounding and reverse causation. Dr. Jose Florez and colleagues avoided these issues by using a bidirectional Mendelian randomization study to test the carbohydrate-insulin model of obesity. They assessed (1) whether a set of genetic variants associated with increased glucose-stimulated insulin secretion predict obesity and (2) whether a separate set of genetic variants associated with obesity predict increased glucose-stimulated insulin secretion. Single nucleotide polymorphisms (SNPs) that predicted higher 30-minute insulin secretion during glucose tolerance testing were significantly associated with higher body mass index (BMI), whereas and SNPs that predicted BMI were not significantly associated with higher observed 30-minute insulin. These results support the carbohydrate-insulin model of obesity by demonstrating that randomly assigned SNPs that predict higher insulin secretion appear to be causally associated with higher observed BMI.
Citation:
Genetic Evidence That Carbohydrate-Stimulated Insulin Secretion Leads to Obesity.
Astley CM, Todd JN, Salem RM, Vedantam S, Ebbeling CB, Huang PL, Ludwig DS, Hirschhorn JN, Florez JC. Clin Chem. 2018 Jan;64(1):192-200. doi: 10.1373/clinchem.2017.280727. PMID: 29295838
Research Details:
- Research Center: Harvard Medical School
- Featured NORC Members: David S. Ludwig, MD, PhD, Professor of Pediatrics, Boston Children’s Hospital and Harvard Medical School; Joel Hirschhorn, MD, PhD, Professor of Pediatrics, Boston Children’s Hospital and Harvard Medical School; Jose Florez, MD, PhD, Associate Professor of Medicine, Massachusetts General Hospital and Harvard Medical School
- Center contributions: Drs. Ludwig, Hirschhorn, and Florez are members of the NORCH.

